
Key Takeaways
- Sleep apnea is a significant, often overlooked, cause of chronic high blood pressure.
- The "non-dipping" blood pressure pattern, where blood pressure doesn't drop at night, is a strong indicator of underlying sleep apnea.
- Resistant hypertension, uncontrolled by multiple medications, is highly correlated with undiagnosed sleep apnea.
- Early identification and treatment of sleep apnea can lead to improved blood pressure control and reduced cardiovascular risks.
- Frontier Sleep & Wellness offers accessible, medical-grade home sleep testing to uncover these hidden connections.
The Hidden Connection: Is There a Link Between Sleep Apnea and High Blood Pressure?
For millions of people, managing high blood pressure (hypertension) is a daily routine of medication and lifestyle adjustments. Yet, what if the root cause isn't just diet or genetics but something that happens every night during sleep? There is a powerful and often-overlooked link between obstructive sleep apnea (OSA) and chronic hypertension. Many individuals diligently treat their high blood pressure without ever addressing this critical underlying factor, leaving them with persistent cardiovascular strain and unresolved health risks. Untreated sleep apnea can be the missing piece of the puzzle for those struggling to get their blood pressure under control.
How Sleep Apnea Elevates Your Blood Pressure
The relationship between sleep apnea and high blood pressure isn't coincidental; it's a direct physiological response to the stress the disorder places on your body. When you have OSA, your airway repeatedly closes during sleep, causing you to stop breathing for seconds or even minutes at a time. These episodes trigger a cascade of emergency responses that, night after night, lead to a chronic state of hypertension.
The Role of Oxygen Deprivation and Stress Response
Each time you stop breathing, the oxygen level in your blood drops, a condition known as intermittent hypoxia. Your brain recognizes this as a life-threatening event and jolts your body into action. It activates the sympathetic nervous system, the body's "fight or flight" mechanism, which releases stress hormones like adrenaline. This hormonal surge causes your heart to beat faster and your blood vessels to constrict, leading to an immediate spike in blood pressure to restore oxygen flow. When this cycle repeats dozens or hundreds of times per night, it keeps your cardiovascular system in a constant state of high alert, preventing it from resting and leading to sustained high blood pressure during the day.
Inflammation and Vascular Damage
The consequences of sleep apnea extend beyond immediate stress responses. The chronic cycle of oxygen drops and surges contributes to systemic inflammation and oxidative stress throughout the body. This ongoing inflammation can damage the delicate lining of your blood vessels (the endothelium), making them stiff and less flexible. This loss of elasticity, or arterial stiffness, means your heart has to work harder to pump blood, further contributing to chronically elevated blood pressure and increasing your long-term cardiovascular risk.
Understanding "Non-Dipping" Blood Pressure
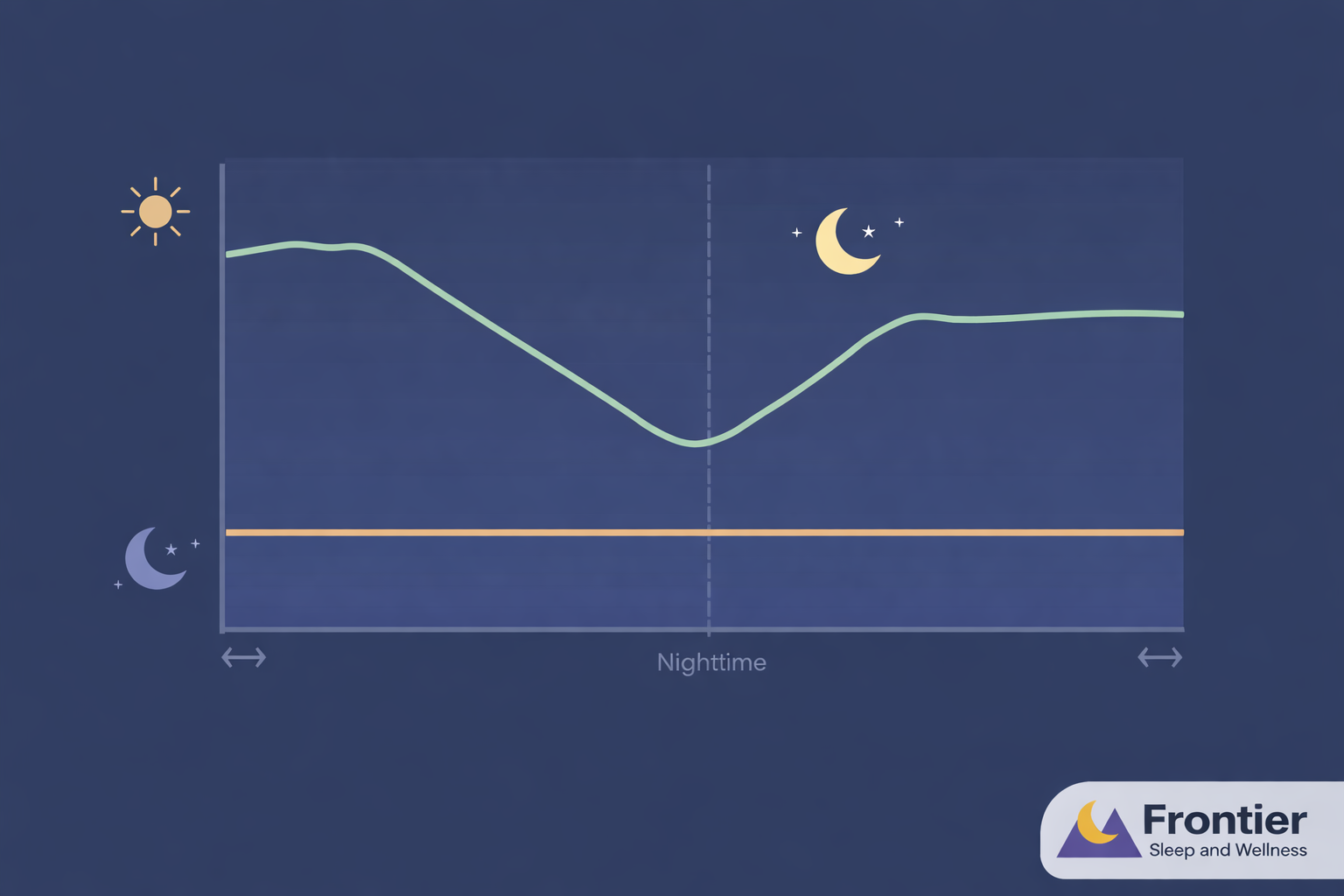
In a healthy individual, blood pressure follows a natural circadian rhythm. During the day, it's higher, and at night, during restful sleep, it should decrease by 10-20%. This healthy nocturnal drop is known as "dipping." However, in many people with untreated sleep apnea, this crucial dip doesn't happen.
A "non-dipping" pattern is when your blood pressure remains elevated, or in some cases, even rises, during the night. This is a significant red flag for underlying health issues, including OSA. The continuous strain on your cardiovascular system from a non-dipping pattern is a major concern, as nighttime blood pressure is a powerful predictor of cardiovascular events like heart attack and stroke, independent of daytime readings. This lack of nocturnal rest for your heart and arteries significantly accelerates wear and tear on the entire system.
Resistant Hypertension: A Strong Indicator of Sleep Apnea
For some, high blood pressure becomes exceptionally difficult to manage. Resistant hypertension is formally defined as high blood pressure that remains above target levels despite the use of three or more different classes of antihypertensive medications, including a diuretic. If you and your doctor are struggling to control your blood pressure with multiple medications, there is a very strong possibility that undiagnosed sleep apnea is the culprit.
Studies have shown an incredibly high prevalence of OSA in patients with resistant hypertension, with some estimates suggesting it affects 70-85% of this group. In fact, OSA is considered the most common secondary cause of resistant hypertension. The constant activation of the sympathetic nervous system caused by sleep apnea directly counteracts the effects of many blood pressure medications, making them less effective. This makes a sleep apnea diagnosis a critical step in managing hard-to-control hypertension.
Key Symptoms & Warning Signs: When High Blood Pressure Suggests Sleep Apnea
If high blood pressure is your primary health concern, it's easy to overlook other symptoms. However, when combined with hypertension, the following warning signs create a compelling case for considering a sleep apnea evaluation:
- Loud, persistent snoring: Often the most obvious sign reported by a partner.
- Daytime fatigue or sleepiness: Feeling tired despite a full night's sleep.
- Morning headaches: Waking up with a headache that dissipates during the morning.
- Nocturia (frequent nighttime urination): Waking up multiple times to use the bathroom.
- Brain fog or difficulty concentrating: Struggling with memory or focus during the day.
- Observed pauses in breathing: A partner may notice you stop breathing, gasp, or choke during sleep.
If you are being treated for hypertension and experience any of these symptoms, it's a strong signal that your sleep should be investigated.
When to Consider a Sleep Apnea Test
Making the decision to get a sleep test is a proactive step toward better cardiovascular health. You should strongly consider a diagnostic evaluation if you have:
- Resistant Hypertension: Your blood pressure remains high despite taking three or more medications.
- A "Non-Dipping" Blood Pressure Pattern: Confirmed through 24-hour ambulatory blood pressure monitoring.
- Hypertension Combined with Snoring and Fatigue: The classic combination of symptoms.
- Worsening Morning Blood Pressure: Your readings are consistently highest upon waking.
Why Act Early? The Benefits of Timely Diagnosis
Early diagnosis and treatment of sleep apnea can do more than just improve your sleep—it can be life-changing for your cardiovascular health. By addressing the root cause, you can prevent or mitigate long-term damage to your heart and blood vessels. Effective treatment can improve the efficacy of your blood pressure medications, potentially reduce the number of medications you need, and lower your overall risk for heart attack, stroke, and kidney damage.

The Impact of Treating Sleep Apnea on Blood Pressure
Treating sleep apnea directly addresses the intermittent hypoxia and stress responses that drive up blood pressure. By keeping the airway open throughout the night, treatments restore normal oxygen levels and allow the nervous system to rest. This leads to significant improvements in blood pressure control for many patients.
Effective treatment options work by preventing the airway collapse that triggers the "fight or flight" response. Continuous Positive Airway Pressure (CPAP) therapy uses pressurized air to keep the airway open. For those seeking CPAP alternatives, Oral Appliance Therapy (OAT) offers a comfortable and effective solution by repositioning the jaw to maintain an open airway. By managing the underlying sleep disorder with a custom oral device, patients often see a stabilization of their blood pressure, a reduction in cardiovascular strain, and an overall enhancement in their quality of life.
How Frontier Sleep & Wellness Empowers Your Health Journey
At Frontier Sleep & Wellness, we understand the critical link between sleep quality and cardiovascular health. We are dedicated to empowering patients in San Antonio, South Austin, and surrounding Texas communities to take control of their well-being. We simplify the diagnostic process with convenient, medical-grade home sleep testing, eliminating the need for an overnight stay in a lab while providing clinically accurate results. To understand the investment, you can learn about the costs of sleep tests upfront.
Our patient-centered approach emphasizes treatment freedom. We work collaboratively with your primary care physician and specialists in cardiology to ensure your sleep health is an integral part of your overall care plan. Whether it's CPAP or a comfortable alternative like OAT, our goal is to find the right solution for you. If you have more questions, please visit our FAQs page, contact us, or get an appointment today to start your journey toward better sleep and better blood pressure control.
FAQs
What is non-dipping blood pressure?
Non-dipping blood pressure refers to a pattern where an individual's blood pressure does not decrease by the usual 10-20% during nighttime sleep, which is a normal physiological process. This sustained elevation during rest is often associated with underlying health issues, including sleep apnea, and can increase cardiovascular risk.
What is resistant hypertension?
Resistant hypertension is defined as high blood pressure that remains elevated and uncontrolled despite treatment with at least three different classes of antihypertensive medications, ideally including a diuretic, at their maximum tolerated doses. It is strongly linked to conditions like undiagnosed sleep apnea.
Should people with high blood pressure get tested for sleep apnea?
Yes, people with high blood pressure should consider getting tested for sleep apnea, especially if they exhibit symptoms like loud snoring, daytime fatigue, or if their hypertension is resistant to medication or shows a "non-dipping" pattern at night. Identifying and treating sleep apnea can significantly improve blood pressure control.
Can treating sleep apnea improve blood pressure?
Yes, treating sleep apnea can often lead to improved blood pressure control. By addressing the root cause of nocturnal oxygen drops and stress responses, treatments like oral appliance therapy or CPAP can help stabilize blood pressure, reduce medication reliance in some cases, and lower the overall risk of cardiovascular complications.






.png)
